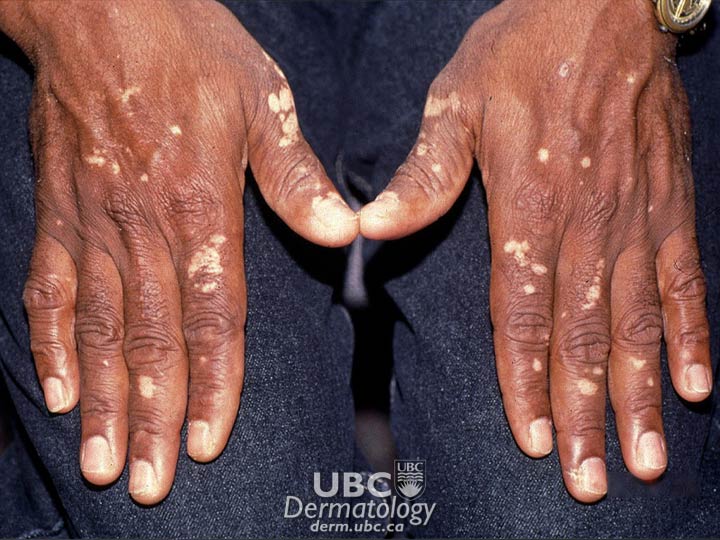
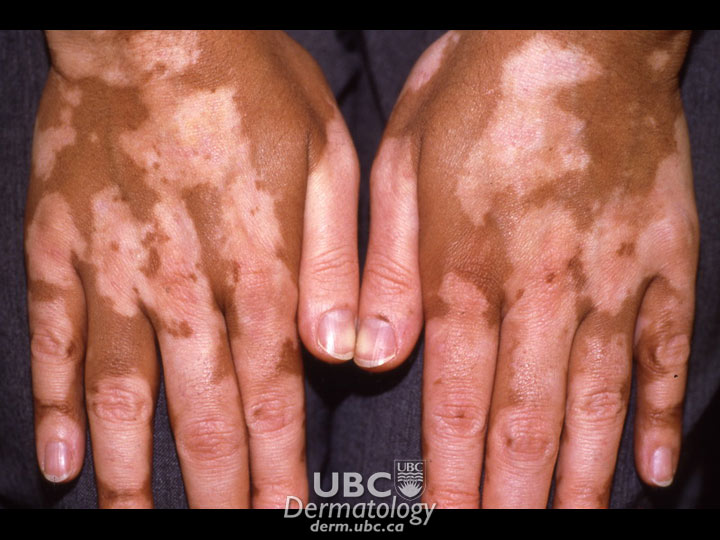
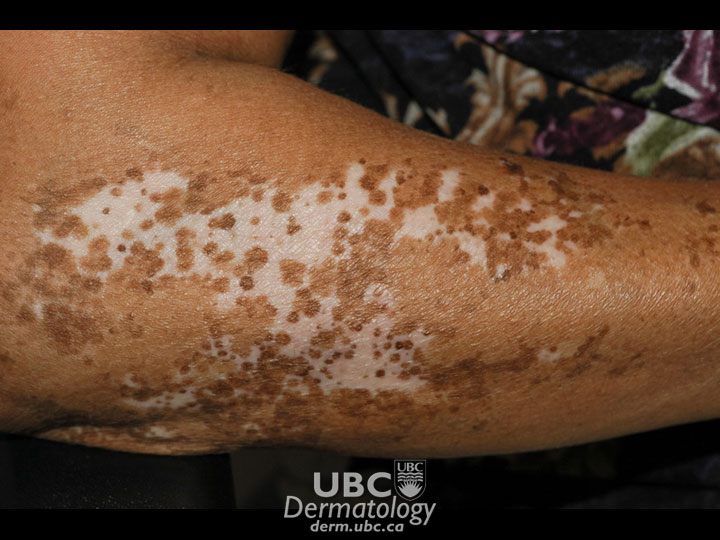
Diagnosis is by physical examination, medical history, and laboratory tests.
Physical Exam
A doctor will confirm the presence of white patches on the skin in expected areas in one of the three typical patterns. A Woods’ Lamp, which shines ultraviolet light onto the skin, is frequently used to examine areas, as vitiligo glows under this type of light.
Medical History
Your family doctor will ask you if you:
- or any family member have an autoimmune disease
- have had a rash, sunburn, or other skin problem before the appearance of the white patches
- have suffered recent stress or illness
- have greyed before the age of 35
- are sensitive to the sun
Laboratory Tests
Your doctor may occasionally need to take a skin sample, but most cases of vitiligo can be diagnosed by direct visual examination. Skin affected by vitiligo shows no pigment-producing melanocytes. Blood tests may also be done to rule out pernicious anemia, thyroid disease or another autoimmune disease.
Treatment
Vitiligo cannot be cured, but treatments are available that might even out skin colour. Fair-skinned patients with a few small patches may choose not to treat vitiligo, and sunscreen and cosmetics may be all that is needed to camouflage the patches. Vitiligo can be disguised with a variety of make-up or a homemade stain made from food colouring and rubbing alcohol, although commercially available products give a more natural skin colour match.
Children can be treated with topical steroids, topical immunomodulators, or narrowband ultraviolet B (UVB) light treatment; they frequently repigment faster than adults, so catching it early can make it easier to treat before patches become larger and more numerous.
Patients with darker skin or those with patches that are large or great in number may opt for medical treatment to either restore white patches to their original colour (repigment) or destroy remaining colour to match the white patches (depigment). Some commonly used treatments are described below.
Topical Corticosteroid Therapy
Corticosteroid creams can return colour to the skin, particularly if applied at an early stage. A mild topical cream or ointment may be prescribed for young children (under 10 years) while adults use a stronger form. Treatment is simple—the cream or ointment is applied to the white patches—but monitoring must be conducted for side effects such as skin thinning or streaking. Corticosteroids may be used along with a topical vitamin D derivative. Results may be seen after three months but are not as effective as psoralen photochemotherapy (see below).
Topical Immunomodulator Therapy
A relatively new treatment for vitiligo uses topical immunomodulators, such as tacrolimus and pimecrolimus, which work to regulate the local immune system activities that result in depigmentation. They are now commonly prescribed by dermatologists for facial and other areas and can be used for longer periods without the side effects of corticosteroids. Side effects include transient burning and stinging sensations in the skin and a potential increased risk for cancer, although this is considered extremely rare.
Narrow-band Ultraviolet B (NB-UVB) Therapy
Narrow-band UVB therapy is an alternative to UVA therapies. Narrow-band UVB light is administered up to three times a week without pre-application of psoralen. This treatment is simpler and may be safer than previous forms of ultraviolet therapies. Studies have shown that it is now considered the treatment of choice for vitiligo covering more than 10-20 per cent of the body.
Depigmentation
Depigmentation involves fading normal skin to match the already white areas, an option that may be considered if vitiligo affects more than 50 per cent of the body. Monobenzylether of hydroquinone (monobenzone) is applied twice daily to pigmented areas until they match depigmented areas. However, there are a number of adverse effects. Major side effects include redness and swelling of the skin and permanent sun sensitivity. Other side effects are itching, dry skin, and abnormal darkening of the membrane covering the whites of the eyes. Depigmentation is permanent and irreversible and patients need to think carefully before pursuing this option.
Transplant Surgery
Only a small percentage of patients are eligible for vitiligo skin transplant surgery. Three options for surgical treatment are available:
- “Minipunch” skin transfer: This method uses the person’s own tissue to treat small patches. Small pieces of normal skin are removed and attached to depigmented sites. Possible complications include infection at donor or recipient sites (rare), scarring, a cobblestone skin texture, spotty pigmentation, and vitiligo appearing at the donor site due to skin trauma.
- Blister grafting: This process uses heat, cold or suction to produce blisters over pigmented and depigmented skin. The tops of the pigmented blisters are removed and transplanted to the depigmented skin areas. The risks are scarring and a cobblestone appearance.
- Autologous melanocyte transplant: In this procedure, a sample of normal pigmented skin is isolated in a laboratory dish containing a special cell suspension solution. Once enough melanocytes have been isolated, they are transplanted to depigmented areas of the skin.
Tattooing (micropigmentation)
In this method, pigment is inserted into the skin. It has proven to be most effective in the lip area in dark-skinned people. Disadvantages are that it is difficult to match natural skin colour and any tattooing can fade with time. A possible side effect in the lip area is that it may lead to blisters caused by the herpes simplex virus in people already infected with the virus. Side effects in other areas are that it may cause vitiligo to spread in the tattooed area due to skin trauma. Finally, tattooing is not reversible, since tattoos used for micropigmentation cannot be safely removed by laser technology. Generally, this treatment is not recommended in most cases.
Research on vitiligo is ongoing and includes a number of studies exploring the role of skin trauma as well as the identification and analysis of genes that may cause or contribute to the condition. Researchers may be testing new medications for vitiligo as part of these research studies.
*All information on medical treatments on this site is provided as an overview only. For a complete and up-to-date list of side effects, warnings and precautions, read the product’s package insert and consult your doctor or a pharmacist.
**If you are considering an alternative or complementary therapy, discuss it with your doctor first, and always be sure to keep your doctor up to date about any vitamins, supplements, or other forms of alternative treatment you are taking. Like any medication, alternative therapies can interact with other medications/treatments and, in some cases, have side effects of their own. Remember that “natural” does not necessarily mean “safe.”
 Vitiligo Voices Canada (VVC) is a non-profit organization.
Vitiligo Voices Canada (VVC) is a non-profit organization.