Coping and Support
Atopic dermatitis has been called the condition you “wear” as it affects your appearance. And while the clinical aspects of atopic dermatitis are obvious, the psychological effects may not be. Symptoms such as redness and flaking can be severe and, when visible to others, can cause some people to be self-consciousness. As well, friends, family and colleagues may not understand this condition, and their lack of sensitivity may upset those with atopic dermatitis.
In addition, the pain and itching associated with atopic dermatitis can be a particular problem at night when it disrupts sleep. Lack of sleep can have repercussions for daily life and interfere with the ability to function well mentally at work or school.
School children particularly may feel embarrassed if they are teased by their classmates because of their condition. As a result, they can experience isolation, low self-esteem, and poor school performance. Parents must be aware of these risks and encourage their children to understand their eczema, be comfortable with it, and talk to their peers about it.
Acknowledging that you have eczema and that it will likely be part of your life for a long time is an important step to managing your well-being. In addition, learning how to control symptoms and keep flare-ups in check through a simple daily skin-care routine can help ease your stress.
Here is a link to a recent report (The Skin I'm in: A NATIONAL REPORT OF THE PATIENT AND CAREGIVER EXPERIENCE WITH ATOPIC DERMATITIS) that we completed in 2017 on the patient and caregiver experience with atopic dermatitis.
Other associations can also help. Visit theEczema Society of Canada or the National Eczema Association (NEA) websites for news, information and advice.
Overview: What is Atopic Dermatitis
The information in this section has been gathered from existing peer-reviewed and other literature and has been reviewed by expert dermatologists on the CSPA Medical Advisory Board.
Atopic Dermatitis, also called Eczema, is a term used to describe a group of persistent or chronic conditions that cause inflammation of the upper layers of the skin. It is usually itchy.
Atopic Dermatitis is activated by the immune system and, despite its sometimes unsightly appearance, is not contagious—but it can flare up repeatedly over the course of someone’s life due to triggers such as illness, stress and exposure to allergens and skin irritants. There are four common types of Atopic Dermatitis or eczema:
Atopic eczema (or atopic dermatitis) may have a genetic component and tends to be found in families with a history of hay fever and asthma. It usually appears on the face, scalp, neck and on the side of the limbs in infants, as well as inside the elbows and behind the knees in older children and adults.
Contact dermatitis occurs in two forms: allergic and irritant. Allergic contact dermatitis is usually a delayed reaction to an allergen, such as poison ivy. Irritant contact dermatitis is more common and is the result of a reaction to an irritant. For example, sodium lauryl sulfate (found in some personal care products such as shampoo, soaps and toothpastes) is one of many solvents that can cause skin irritation.
Xerotic eczema, also known as winter itch, begins as dry skin, usually on the limbs and trunk, and becomes so severe it turns into eczema. This condition occurs most commonly in the elderly, but young people can also develop it.
Seborrhoeic dermatitis is often referred to as dandruff, or cradle cap in infants, and affects the scalp and eyebrows and at times along the sides of the nose.
There are other, less common, forms of Atopic Dermatitis as well:
- Dyshidrosis is typically seen on the palms, soles of feet and sides of fingers and toes. It is characterized by tiny fluid-filed blisters (vesicles), thickening and cracks that itch, especially at night. Warm weather and stress make the condition worse.
- Discoid eczema most frequently appears on the lower legs as round patches of dry, cracked skin that sometimes oozes fluid. The cause is unknown.
- Venous eczema, or stasis dermatitis, is most commonly seen in people over 50 with poor circulation, varicose veins and edema (swelling). It is characterized by redness, itching, and darkening of the skin.
- Autoeczematization, or “ids,” usually occurs as a result of an infection by parasites, fungi, bacteria or viruses and always develops some distance from the initial infection. The type of infection that causes this condition determines how it looks, so the appearance of autoeczematization varies. The only way to cure it is by eradicating the initial infection.
- Neurodermatitis develops when persistent scratching irritates the skin. It is thought to have emotional or “nervous” causes. This condition is controlled with antihistamines and corticosteroids as well as behaviour modification (e.g., learning to stop habitual scratching).
Fast Facts
- Atopic Dermatitis is one of the world’s most frequently diagnosed skin conditions.
- It is particularly common in young children and infants: 10 to 15 per cent of Canadian children under 5 are affected.
- Though some infants outgrow the condition by their second birthday, 40 per cent live with it throughout adulthood.
- About 10 to 20 per cent of the population lives with Atopic Dermatitis in one form or another.
- The number of people with Atopic Dermatitis in Canada is higher than the worldwide average.
Looking Deeper
There are two theories about the causes of Atopic Dermatitis. The first is that a person with atopic dermatitis is predisposed to excess inflammation. This is caused by the type of inflammatory cells present in the skin, the types of chemicals these cells make, and the way they communicate with other cells. The excess inflammation caused by these cells and their chemicals leads to itchy, red, swollen skin, which sets the stage for irritation and infection. The second theory is that a person with atopic dermatitis has skin that does not provide the same protection as a healthy person’s skin. This allows foreign molecules to gain entry to the skin’s deeper layers, provoking inflammation, which causes skin itching and redness. Both theories are most likely interlinked. The causes of atopic dermatitis are still not fully understood; fortunately, international and Canadian dermatology researchers continue to work on this puzzle.
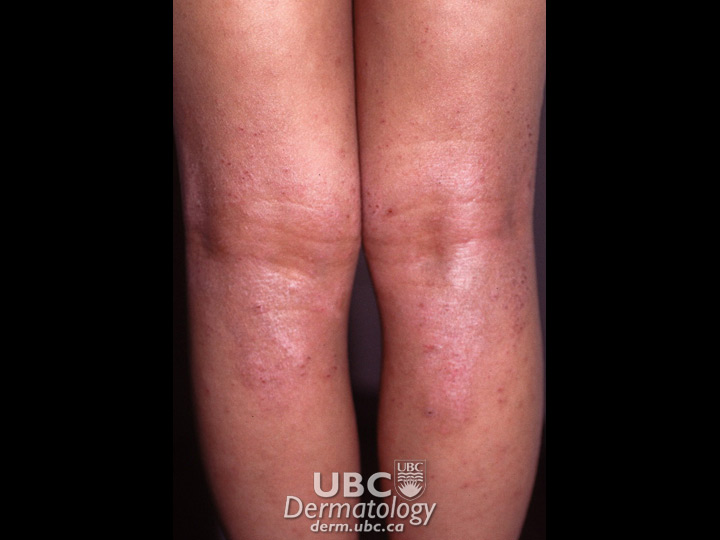 atopic dermatitis-1
atopic dermatitis-1 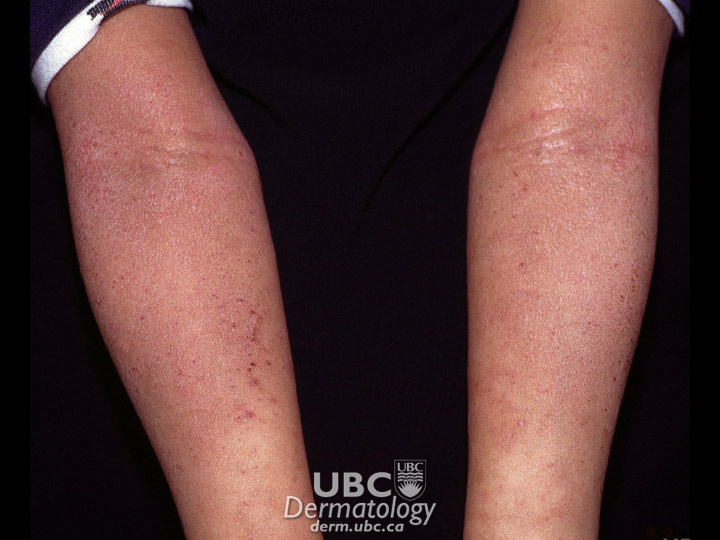 atopic dermatitis -2
atopic dermatitis -2 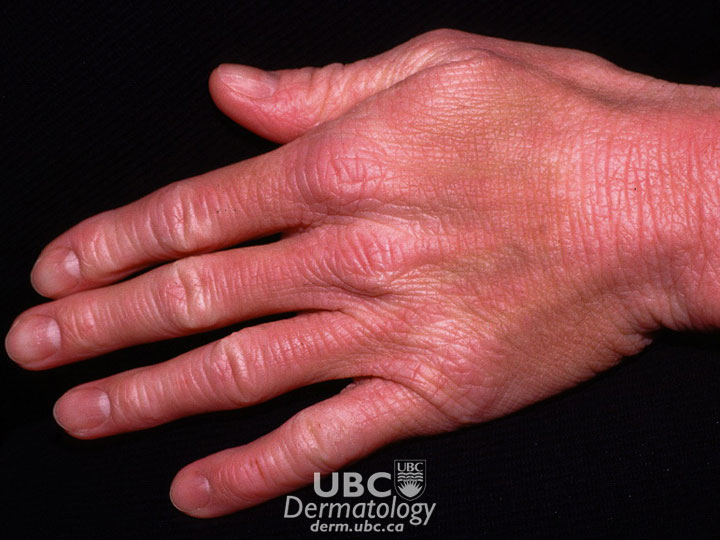 atopic dermatitis-3
atopic dermatitis-3 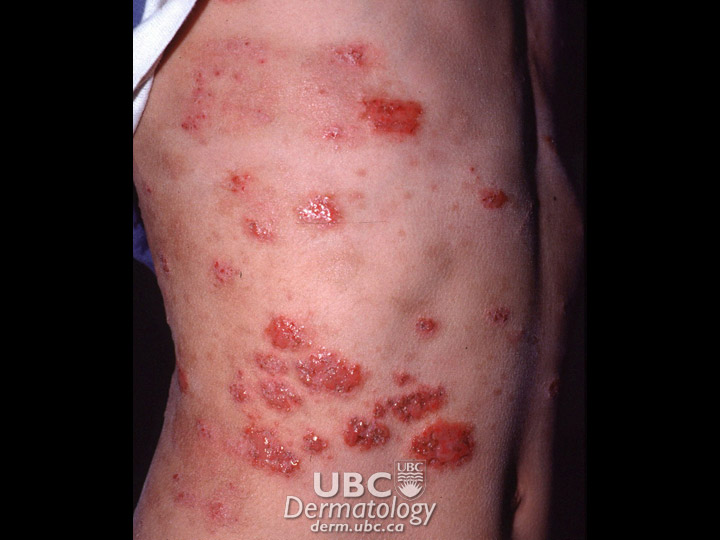 atopic dermatits-4
atopic dermatits-4
Diagnosis and Treatment
Learning the cause of atopic dermatitis isn’t always easy due to the number of possible triggers and the many types of the condition. However, in all cases, a doctor will use the location of the initial rash as a first clue.
For contact dermatitis, a doctor may perform patch testing, which consists of placing small patches on the skin. These patches contain substances typically known to cause the condition. This type of testing can be difficult to interpret as doctors need to select which substances to test, and the results may not always be accurate.
With atopic dermatitis, a physician will explore your medical history and often whether your family members have allergies. This will help identify possible triggers.
For neurodermatitis, your doctor will look to discover any underlying psychological stressors, allergies, or, depending on the rash location, other underlying medical conditions, such as fungal infections, warts or psoriasis.
Although no cure exists for atopic dermatitis, a number of treatment options are available for relieving the inflammation and itching that it causes. The treatments range from lifestyle changes and skin-care strategies to medication.
Lifestyle changes and skin-care strategies
Keeping your skin hydrated is one way to control atopic dermatitis. It is best to hydrate when you wash because bathing allows rough skin to soften, take in water, and better absorb the topical treatments you apply. When bathing or showering, use lukewarm water (not hot). After bathing or showering, lightly pat your skin with a towel. Then apply your prescription ointments or creams and, once they’ve been absorbed, a good moisturizer.
There are many classes of moisturizers. The least effective are lotions or creams; the most effective moisturizers are ointments. It’s usually best to use ointment-type moisturizers during a flare-up and only after you've applied your prescription ointment. When the skin is clear, you can move back to a fragrance-free lotion.
Short, frequent, gentle bathing or showering also washes away Staphylococcus aureus, a bacterium that is found on everyone’s skin and seems to be attracted to atopic dermatitis. Some people with atopic dermatitis can also develop an allergic reaction to this bacterium, which can worsen their condition.
Preventing flare-ups is another effective way to control the condition. Here are some tips to help you to avoid triggering symptoms:
|
AVOID |
INSTEAD |
|
|
Medical Treatments
Treatments for atopic dermatitis generally fall into two categories: those that control symptoms such as itching or dryness, and those that modify the immune system or decrease inflammation. Proper skin care and over-the-counter treatments, as described above, may be enough to control mild cases of atopic dermatitis. If these fail, your doctor may prescribe a topical treatment, such as a medicated cream or ointment, for moderate atopic dermatitis, or a systemic treatment (in pill form) for severe or widespread cases.
Topical treatments (creams, lotions, ointments)
Calcineurin inhibitors are found in creams or ointments containing tacrolimus or pimecrolimus, both of which are immune-modifying drugs. These drugs work by reducing inflammation in the skin. A thin layer of the cream is applied to the affected area twice daily. To avoid rare side effects, these products should not be used continuously over a long period of time, or in children under age 2. You should also minimize exposure to natural (e.g., sunshine) and artificial (e.g., tanning beds) ultraviolet light. Common side effects include a burning feeling or warmth at the application site, which is of short duration and usually disappears after the first week of use.
Corticosteroids are synthetic versions of hormones made in the body. When applied to the skin, they reduce inflammation in the area, making them useful treatments for some forms of atopic dermatitis. Apply the cream sparingly to the affected skin with a gentle massage, 3-4 times each day. Decrease or discontinue the use once the condition is under control. Side effects include dryness, itching, burning and local irritation. Excessive use of corticosteroids (i.e., for an extended period of time over a large area of skin) may cause hormonal problems in rare cases. It is important to follow any instructions your doctor gives you.
Emollient creams/ointments are over-the-counter topical products used to soften and moisturize the skin and help preserve its function as a barrier to water loss. These products may be soothing and help remove dry, scaling skin, as well as increase the effectiveness of other topical treatments. These can be applied generously to affected and unaffected areas.
PDE4 inhibitors are enzymes that help to regulate inflammation in your body. When you have atopic dermatitis, PDE4 enzymes may be overactive in your skin cells. This can lead to inflammation of the skin. The only approved drug of this type is Eucrisa (crisaborole), the first topically applied PDE4 inhibitor to be approved by Health Canada for use for adults and kids as young as 2 years old living with atopic dermatitis. It was developed as a small-molecule, boron-based, selective PDE4 inhibitor that can be used topically. Unlike PDE4 inhibitors that act systemically, this treatment does not cause significant gastrointestinal adverse effects. The most common side effect is stinging and burning when the product is applied to the skin.
Systemic treatments (for very severe atopic dermatitis)
Corticosteroids can also be injected. When taken in this manner, they alter the body’s immune response, reducing inflammation in the skin and elsewhere. As with the topical creams, corticosteroids can cause changes in the body’s hormone production if used excessively. Your doctor will carefully plan the dosing and duration of treatment to avoid this. Less severe side effects include weight gain, nausea or vomiting.
Cyclosporin, a drug used to treat people who have had transplants, has been shown to be effective in people with severe atopic eczema, especially where their lives are significantly disrupted by their condition. The drug is believed to work by suppressing severe allergic and immune reactions. Since it is very powerful, it tends only to be prescribed for a small percentage of patients.
In addition to the medications described above, new treatments not yet on the market are being tested regularly.
Biologics
Biologics (or biosimilars) are medications that are produced from living cells, such as animal cells, bacteria, or yeast. They target specific parts of a person’s immune system to treat diseases such as psoriasis, psoriatic arthritis, rheumatoid arthritis, and some cancers. People can receive biologics through an injection or an intravenous (IV) infusion. The approved drugs for this type of treatment include: Dupixent (dupilumab) and Ebglyss (lebrikizumab) for adult patients living with moderate to severe atopic dermatitis. Common side effects include cold sores, dry eyes and redness at the injection site.
Other Treatments
Medications officially approved for treating other conditions/diseases have been tried in eczema with variable success. They are included here for information only.
Phototherapy is a treatment in which the skin is exposed to ultraviolet light, slowing the growth of affected skin cells. There are two forms commonly used to treat severe atopic dermatitis :
- PUVA (psoralen/ultraviolet A): a drug called psoralen is given (either as pills or applied to the skin) that sensitizes the skin cells to ultraviolet A light. Psoralen pills can cause nausea, vomiting, headaches and sensitivity to UV light (including sunlight)
- UVB (ultraviolet B): uses ultraviolet light (B form) only
Both types of phototherapy are performed at your doctor’s office. As with repeated exposure to natural UV light from the sun, repeated use of phototherapy over a long period of time can lead to drying and ageing of the skin and may increase the risk of skin cancer.
Wet wraps
Wet wraps are a treatment that uses a low-potency topical steroid and an emollient (moisturizer) to calm flares and improve the effectiveness of the medication. It is often used for those with moderate-to-severe atopic dermatitis, especially children, where topical applications have not helped. Wet wraps involve double layers of tubular bandages forming a body suit. They work in two ways:
- Evaporation cools the skin, reducing itching and discomfort. If the bandages become dry, you can remoisten them (this is usually only needed for an overnight treatment).
- Rehydration puts moisture back into the skin as the skin absorbs large amounts of the product. It also improves the penetration of the medication into the skin.
How to perform a wet wrap:
- Cover your chair or sofa with plastic or a garbage bag. Make sure to have a TV or good book within reach!
- Moisten a cloth with room temperature water, wring it out, and set aside. For small treatment areas you can use a washcloth; an old t-shirt or an old pair of long-sleeved and long-legged pyjamas work well for larger areas. Tubular sleeves work as well if you have them.
- Generously apply the prescribed medicated ointment or cream to the affected areas.
- Wrap the areas with the damp clothing/towel, make yourself comfortable with a large blanket, and leave the wrappings for at least 1 hour – it can even be done overnight.
- Remove the coverings and immediately apply a generous amount of an unscented moisturizer all over the body.
- Ideally, continue the procedure twice a day to get flare-ups under control.
Coal tar applied to affected areas has been shown to help reduce the itchiness of atopic dermatitis. But its strong smell and tendency to stain any fabric it touches make it a less appealing remedy. Coal tar can also irritate the skin in some people. It should only be used under the guidance of a doctor with experience in managing atopic dermatitis.
*All information on medical treatments on this site is provided as an overview only. For a complete and up-to-date list of side effects, warnings and precautions, read the product’s package insert and consult your doctor or a pharmacist.
**If you are considering an alternative or complementary therapy, discuss it with your doctor first, and always be sure to keep your doctor up to date about any vitamins, supplements, or other forms of alternative treatment you are taking. Like any medication, alternative therapies can interact with other medications/treatments and, in some cases, have side effects of their own. Remember that “natural” does not necessarily mean “safe.”
Signs and Symptoms
Slightly different symptoms and clinical signs exist for each type of atopic dermatitis, and they can range in terms of severity and location on the body. However, the first symptom of atopic dermatitis is usually intense itching, followed by a patchy, flaky, scaly, dry, hot, inflamed skin rash. Other atopic dermatitis symptoms and clinical signs include:
- Repeated rashes
- Redness
- Swelling
- Crusting
- Scabbing
- Blistering
- Cracking
- Oozing
- Bleeding
As there are different types of atopic dermatitis, so too are there different triggers, which can range from chemicals, bacteria, allergens, side effects of medications and psychological factors. Some triggers include:
- Soaps and detergents
- Cosmetics
- Weather conditions (heat, cold, humidity, dryness)
- Environmental allergens (such as poison ivy, ragweed, and primrose)
- Jewellery
- Creams
- Food handling
- Clothing (due to the chemicals used in manufacturing)
- Sweating
- Gloves
- Rubbing
- Emotional or mental stress
Flare-ups can be caused by:
- Illness
- Unusual physical or mental stress
- Exposure to skin irritants
- Skin infections











