Overview: What are nail disorders?
The information in this section has been gathered from existing peer-reviewed and other literature and has been reviewed by expert dermatologists on the CSPA Medical Advisory Board.
Nail disorders refer to changes in the appearance or condition of healthy nails, which are smooth and hard with an even colour. Irregularities such as white spots or vertical ridges on a nail’s surface are harmless.
In some cases, nail disorders are considered minor yet may require treatment as they can affect everyday tasks such as walking, holding objects, and fastening buttons. However, it is important to note that changes to nails may also signal significant damage to the nail and surrounding tissue, or a more serious underlying disease that requires a visit to the doctor. For example, a red nail bed can indicate the presence of an underlying heart condition, and thick yellow nails can signify lung disease. Generally, you should visit your doctor if you notice any of the following in your nails: changes in colour or shape, swollen skin or pain, white or black lines, or dents or ridges.
The information below focuses on three of the most common nail disorders: onychomycosis, paromychia and ingrown nails.
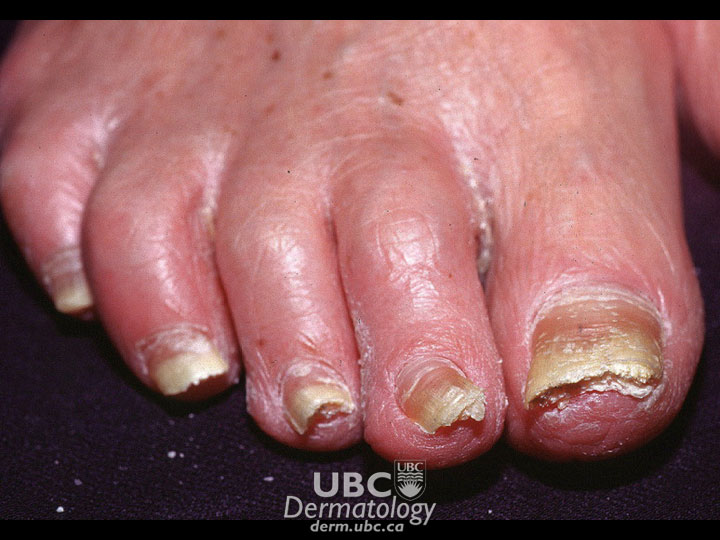
Onychomycosis is caused by fungi, most commonly dermatophytes and less commonly, yeast (Candida). The fungus usually invades the nail at the free edge and then spreads down the side toward the base. Less commonly, it starts from the base and moves upward. Infection may occur in patches or streaks on the nail surface.
Paronychia results when injury to the nail causes the nail to separate from the nail fold and allow the entry of bacteria, most commonly Staphylococcus aureus or Streptococcus species. A mixture of bacteria may be present, particularly in persons with diabetes. Greenish nails suggest Pseudomonas species infection. Chronic paronychia is caused mainly by yeast fungus (Candida).
Ingrown nails occur when the corners or sides of a nail curve and dig into the flesh and an inflammatory response ensues. Ingrown nails may be caused by:
- Improperly trimmed nails (nails should be trimmed square and straight across, to the tip of the toe only using toenail clippers).
- Heredity, which may determine the curvature of nails.
- Tight shoes that crowd the toes.
- Repeated trauma to the feet due to everyday activities.
Coping and Support
Nail disorders generally do not cause as many problems with day-to-day life as other skin conditions. However, ingrown toenails can make walking and running uncomfortable or painful. Paronychia does not normally affect everyday life, but chronic cases may impact some activities. People with the condition may need to break habits such as nail biting or finger sucking to help manage it. Onychomycosis affects people slightly more than the other conditions. It can make walking and typing uncomfortable or even painful. Discoloration and thickening of the nail may be seen as unattractive and therefore embarrassing. In severe cases, the limitations and disfigurement can lead to emotional or psychosocial stress.
Fortunately, people with these conditions can take steps to manage them and prevent them from reccuring. Here are some tips:
Onychomycosis:
- Keep feet clean and dry.
- Avoid nail polish and acrylic nails, which prevent air from reaching the surface.
- Avoid walking barefoot in public showers, pools and locker room areas.
- Change shoes and socks frequently.
- Keep nails clipped short and straight across.
- Wear well-fitting socks and shoes made of breathable materials.
- Disinfect clippers and other instruments used to treat nails.
Paronychia:
- Avoid nail-biting.
- Avoid finger sucking.
- Wear rubber gloves when washing dishes and or performing other activities that require prolonged exposure to water.
- Clean cuts and scrapes promptly to prevent infection.
Ingrown nails:
- After removal of an ingrown nail, follow good nail hygiene practices and choose properly sized footwear.
Symptoms
Onychomycosis
- Possible separation of nail from nail bed
- Buildup of white, green, yellow or black debris under the nail
- Discoloured nail bed and foul odour
- Whitening or yellowing of the nail
- Thickened and crumbling nail
- Numbness, tingling or pain
Paronychia
- Redness, pain and swelling
- Abscesses (pus-filled cavities) may form
- Duration is usually acute but chronic paronychia has symptoms lasting more than six weeks
- Symptoms usually occur at the side of the nail fold
- Occasionally the entire horseshoe of skin around the nail is involved
- Green colouration of the nail indicates a Pseudomonas bacteria infection
Ingrown nails
- Redness, swelling and tenderness
- Pain during walking or running
- Corners or sides of nails digging into soft tissue
Other symptoms can indicate a more serious underlying condition. The following are some common signs to watch for when examining your nails:
|
Nail appearance |
Potential cause |
|
White spots on nail |
Mild trauma; may indicate infection |
|
Thin, reddish-brown vertical lines under the nail |
Damage to blood vessels in nail bed |
|
Clear, jelly-filled bubble at nail base |
Cyst that requires removal |
|
Dark spots, streaks |
Injury; if no injury, melanoma (skin cancer) |
|
Pits, ripples, discoloration; crumbling and separation from nail bed |
Psoriatic nails accompanying psoriasis |
|
White nails |
Liver diseases |
|
Half of nail is pink, other half is white |
Kidney diseases |
|
Thick, yellow nails; slow growth |
Lung disease |
|
Nail bed is red |
Heart conditions |
|
Nail bed is pale |
Anemia |
|
Yellow nails, slightly pink at base |
Diabetes |
|
No nail, thick nail, curved nail |
Congenital deformities |
|
Triangular half-moon at base of nail, thumb nails partially absent |
Nail-Patella Syndrome |
|
Concave, spoon-shaped nail |
Plummer-Vinson syndrome |
|
Rough, pitted opaque nail |
Alopecia areata |
|
Horizontal white lines |
Abnormality in blood vessels beneath nail; may point to other conditions such as pellagra, Hodgkin disease, sickle-cell anemia |
Diagnosis and Treatment
Most nail disorders are diagnosed by a doctor through visual examination. In the case of paronychia, laboratory tests may be, but are rarely, required. In the case of onychomycosis, diagnosis is important, as other nail problems can look similar. Analysis is by microscopic examination or culture of the fungus.
Treatment varies depending on the type of nail disorder.
Onychomycosis
Fungal infections can be difficult to cure, and treatment depends on the severity of the symptoms. Some infections will respond to topical antifungal creams, lotions, gels or nail lacquers. However, most fungal nail infections require treatment with oral antifungal drugs (for example, itraconazole, terbinafine or fluconazole). These drugs may improve the condition and completely cure it; however, the infection often recurs when the drugs are discontinued. In some cases, part of the infected nail may need to be removed to allow direct application of a topical antifungal. This treatment is generally effective only in cases where the infection is superficial. The nail will grow back unless the bed is severly injured. Chronic pain may require permanent removal of the nail. Recently laser therapy has been reported as useful in the treatment of onychomycosis, and currently studies are being done to confirm the exact effectiveness of this therapy
Paronychia
Hot compresses and warm soaks can relieve pain and often drain pus. Sometimes, a doctor will make a small cut into the pocket of infection (abscess) to drain it more quickly and then apply an antiseptic. Nail plate removal may be required if the abscess is under a raised nail. If the doctor suspects the infection is spreading or the condition is caused by a fungus, then she or he may prescribe oral antibiotics.
Ingrown nails
If not severe, the foot may be soaked in warm salt or soapy water followed by placement of dry cotton under the corner of the nail. More severe cases require professional removal of ingrown sides and treatment of any infection, as self-treatment could lead to serious infection, particularly if the toe is sore or an open wound is present. A doctor will usually numb the area with anaesthetic and then remove the ingrown section of the nail. The ingrown nail usually doesn’t recur. Chronic cases require professional removal of ingrown nail and its root by chemical, laser or other methods.
*All information on medical treatments on this site is provided as an overview only. For a complete and up-to-date list of side effects, warnings and precautions, read the product’s package insert and consult your doctor or a pharmacist.
**If you are considering an alternative or complementary therapy, discuss it with your doctor first, and always be sure to keep your doctor up to date about any vitamins, supplements, or other forms of alternative treatment you are taking. Like any medication, alternative therapies can interact with other medications/treatments and, in some cases, have side effects of their own. Remember that “natural” does not necessarily mean “safe.”